_1763966179_WNo_1600d900.jpg)
Table of Content
- Introduction
- Why Do Joints Hurt When the Weather Turns Cold?
- Common Conditions That Get Worse in Cold Weather
- Lifestyle Factors That Make Joint Pain Worse in Cold Seasons
- How to Reduce Cold-Weather Joint Pain
- How Cold Weather Aggravates Different Joints
- Common Symptoms of Cold-Weather Joint Pain
- Conclusion
Introduction
As temperatures begin to drop, many people notice a familiar and uncomfortable sensation: their joints start to feel stiff, achy, or even swollen. This phenomenon is extremely common among individuals with osteoarthritis, rheumatoid arthritis, gout, tendinitis, and people with old joint injuries. However, even healthy individuals may feel increased discomfort in colder seasons, leading many to wonder why joint pain seems to worsen whenever the weather turns chilly.
Cold-weather joint pain is not merely a subjective feeling. A combination of physiological, environmental, and lifestyle factors contribute to joint discomfort as temperatures decline. Changes in barometric pressure can affect the tissues around the joints, colder temperatures can reduce blood flow and increase muscle stiffness, and lower humidity levels may alter how the joint structures behave and respond to force. For people who already struggle with chronic joint conditions, these subtle changes can amplify inflammation or pressure on sensitive nerves, making the pain more noticeable.
In addition to biological factors, daily habits during colder months—such as reduced physical activity, longer periods of sitting indoors, and fluctuations in vitamin D levels—can further aggravate joint discomfort. The colder seasons often bring about lifestyle adjustments that unintentionally put additional stress on the body. For example, decreased mobility leads to weakened supporting muscles, which in turn makes joints work harder than they should.
Understanding why cold weather causes joint pain is the first step toward managing it effectively. With the right strategies—ranging from maintaining proper body warmth, staying active, improving posture, and using high-quality joint support braces—many individuals can minimize seasonal discomfort and maintain a better quality of life. For businesses, physiotherapists, and distributors seeking reliable solutions for joint support products, it is also important to understand how environmental factors influence the demand for specialized braces during colder months.
In the following sections, this comprehensive guide will explain the science behind cold-weather joint pain, common conditions that worsen in low temperatures, practical ways to relieve symptoms, and how professional joint-support products—such as wrist braces, knee braces, shoulder supports, and compression gloves—play a crucial role in managing discomfort during the cold season.
Why Do Joints Hurt When the Weather Turns Cold?

When temperatures begin to fall, the human body undergoes a number of physiological adjustments designed to conserve heat and protect vital organs. While these changes are beneficial for survival, they can also create discomfort in the musculoskeletal system—particularly in weight-bearing or previously injured joints. Below are the primary scientific explanations behind cold-weather joint pain.
1. Barometric Pressure Drops Affect Joint Tissues
One of the most widely recognized reasons for weather-related joint pain is the fluctuation in barometric (atmospheric) pressure. Before a cold front or storm arrives, barometric pressure typically drops. This reduction means surrounding air pressure decreases, allowing body tissues—especially those that are inflamed—to expand slightly.
Although the expansion is small, it increases pressure within the joint cavity and surrounding nerve endings. People with arthritis or joint degeneration often have less cushioning cartilage, making them more sensitive to these micro-pressure changes. As a result, they may experience more stiffness, tenderness, or swelling when the weather cools.
For individuals with chronic joint issues, this barometric sensitivity can be strong enough that they can “predict” changes in weather based on how their joints feel.
2. Lower Temperatures Reduce Blood Circulation
When the weather becomes cold, the body prioritizes keeping the core warm. To do so, it constricts blood vessels in the extremities, including the hands, feet, knees, and elbows. This physiological response—known as vasoconstriction—reduces the amount of warm, oxygen-rich blood that reaches peripheral joints.
Reduced circulation leads to:
-
Slower delivery of nutrients to cartilage and soft tissue
-
Increased stiffness in connective tissues
-
Delayed removal of metabolic by-products
-
A heightened sensation of pain and tightness
This is why individuals often feel their joints become more rigid or sore after being outdoors in cold weather or waking up in a chilly room.
3. Synovial Fluid Thickens in Cold Weather
Synovial fluid is the natural lubricant found inside joints, allowing bones to glide smoothly during movement. However, when temperatures drop, this fluid can become slightly thicker and less viscous.
Thicker synovial fluid means:
-
Joints feel less “oiled”
-
Movements become less smooth
-
Stiffness increases
-
Pain during bending, stretching, or lifting becomes more noticeable
For people with arthritis, already-reduced cartilage and limited joint lubrication make this effect even more pronounced.
4. Muscles Tighten to Preserve Body Heat
Cold temperatures cause muscles to contract and tighten as a protective response, helping the body retain heat. While this is beneficial for temperature regulation, it can create added stress on the joints.
Tight muscles can:
-
Reduce joint range of motion
-
Increase tension on tendons and ligaments
-
Cause surrounding tissues to pull unevenly on joints
-
Lead to soreness, stiffness, and fatigue
This muscle tension often explains why many people experience worsened neck, shoulder, and lower-back pain during cold seasons.
5. Increased Sensitivity of Nerves in Cold Conditions
Cold can heighten nerve sensitivity, especially in areas with inflammation or previous injury. Nerves that are exposed due to cartilage thinning—common in osteoarthritis—can react strongly to temperature drops.
Colder temperatures may:
-
Slow nerve signal transmission
-
Increase perceived pain intensity
-
Aggravate numbness or tingling
-
Trigger sharper or more noticeable discomfort
Individuals with neuropathic conditions may especially feel this amplification.
6. Decreased Physical Activity Contributes to Joint Stiffness
In colder seasons, people are generally less active:
-
Outdoor activities decrease
-
People remain seated for longer hours
-
Muscles become deconditioned
-
Joints stiffen from disuse
Inadequate movement reduces synovial fluid circulation and lowers muscle strength—two factors essential for healthy joint function. Even a temporary reduction in daily activity can make joints feel less stable and more sensitive to temperature changes.
7. Seasonal Mood Changes Affect Pain Perception
Cold seasons, shorter days, and reduced sunlight exposure can influence mood and energy levels. Research suggests that lower serotonin levels and reduced vitamin D synthesis may heighten the brain’s perception of pain.
This emotional component does not cause joint pain directly, but it acts as a magnifier. When combined with physical stressors, individuals may feel joint discomfort more intensely.
Common Conditions That Get Worse in Cold Weather

While cold weather can cause general discomfort for anyone, certain joint-related conditions tend to worsen significantly as temperatures drop. Individuals with pre-existing inflammation, past injuries, or chronic musculoskeletal disorders often experience heightened sensitivity during the winter months or any period of sudden temperature decline. Below are the most common conditions affected by cold weather and why symptoms intensify in these seasons.
Lifestyle Factors That Make Joint Pain Worse in Cold Seasons
While physiological changes caused by cold temperatures play a major role in joint pain, lifestyle habits during colder months can significantly amplify discomfort. Many people unknowingly adopt routines that increase stiffness, reduce circulation, or place unnecessary strain on vulnerable joints. Recognizing these lifestyle factors is essential for managing cold-weather joint pain effectively.
1. Reduced Physical Activity
Cold seasons typically lead to lower levels of physical activity. Shorter daylight hours, decreased outdoor time, and overall reluctance to move in cold environments contribute to a more sedentary lifestyle. Reduced activity can weaken supporting muscles and increase strain on joints, resulting in:
-
Slower synovial fluid circulation
-
Increased stiffness in the morning or after sitting
-
Faster onset of fatigue during small tasks
-
Heavier reliance on joints without adequate muscle support
Over time, even slight reductions in daily movement can cause the joints—especially the knees, hips, neck, and lower back—to feel more painful or less stable.
2. Poor Posture and Prolonged Sitting

Working indoors or staying at home longer during cold seasons often means extended hours sitting at desks, sofas, or beds. Poor posture—such as leaning forward, crossing legs, or slouching—places continuous and imbalanced pressure on the joints and spine.
Common effects include:
-
Neck and shoulder tension
-
Lower-back strain
-
Increased cartilage wear in hips and knees
-
Tightening of surrounding muscles and ligaments
Once the body stiffens in these positions, cold temperatures amplify the discomfort by reducing tissue flexibility.
3. Exposure to Cold Indoor Environments
Many people assume only outdoor temperatures affect their joints. However, cold indoor environments—air-conditioned offices, uninsulated rooms, or first-floor spaces—can have the same impact. Prolonged exposure to low temperatures indoors can reduce circulation, trigger muscle tightening, and increase joint stiffness.
Individuals who work in warehouses, laboratories, logistics centers, or refrigerated environments often experience more intense symptoms.
4. Lower Vitamin D Levels During Cold Seasons
Reduced sunlight exposure in colder months lowers the body’s natural production of vitamin D. This essential nutrient supports bone health, calcium absorption, immune function, and muscle performance. Low vitamin D levels have been associated with increased musculoskeletal pain and heightened sensitivity in joints.
People with deficiency may experience:
-
Increased joint aches
-
Muscle weakness
-
Greater susceptibility to inflammation
-
Slower recovery after physical activity
This is especially common among individuals living in northern regions with limited winter sunlight.
5. Weight Gain and Increased Joint Load
Seasonal changes in diet and reduced movement can contribute to slight weight gain during colder months. Even a small increase in body weight can place additional pressure on weight-bearing joints, particularly the knees, hips, and lower back. For example, each extra kilogram of body weight can translate into several kilograms of added force on the knee joint during walking or climbing stairs.
As a result, colder seasons may trigger a feedback loop: reduced activity → weight gain → increased joint stress → more pain → even less movement.
6. Wearing Non-Supportive Shoes or Clothing
Cold seasons often encourage people to wear heavier clothing and less flexible footwear. Boots with inadequate arch support or stiff soles can affect gait patterns, increasing pressure on the knees, ankles, and hips. Thick but restrictive clothing can also limit mobility, reducing joint warmth and flexibility.
This combination increases the risk of discomfort, especially for individuals with arthritis, tendinitis, or chronic foot and ankle problems.
7. Insufficient Joint Protection During Daily Activities
Without proper support, weakened or inflamed joints must absorb more stress during daily tasks. For individuals with chronic conditions or old injuries, cold weather magnifies this strain. This is why many physiotherapists and orthopedic specialists recommend using professional braces—such as wrist, knee, elbow, or back supports—during colder seasons to stabilize joints and maintain warmth.
This topic leads naturally into the next section.
How to Reduce Cold-Weather Joint Pain
Managing joint pain during cold seasons requires a combination of medical awareness, lifestyle adjustments, and protective strategies. While cold-weather–related joint discomfort is common, many individuals can significantly reduce symptoms by adopting simple habits that support circulation, mobility, and joint stability. The following evidence-based approaches are widely recommended by physiotherapists, orthopedic specialists, and pain-management professionals.
1. Keep the Body Warm at All Times
Maintaining warmth is one of the simplest and most effective ways to reduce joint discomfort. Warmth helps improve circulation, relax muscle tension, and keep synovial fluid at an optimal viscosity.
Effective warming strategies include:
-
Dressing in layers to trap heat
-
Wearing gloves, knee sleeves, or thermal socks in cold environments
-
Using heating pads or warm compresses on stiff areas
-
Taking warm showers before physical activity
People who work in cold indoor environments—such as warehouses or manufacturing sites—should pay special attention to keeping hands, knees, and lower back protected.
2. Stay Active and Avoid Long Periods of Inactivity
Movement is essential for joint health. Even gentle physical activity increases blood flow, activates supporting muscles, and distributes synovial fluid across joint surfaces.
Recommended activities include:
-
Low-impact cardio (walking, cycling, elliptical)
-
Yoga or stretching routines focusing on mobility
-
Light strength training to stabilize joints
-
Short movement breaks every 30–45 minutes if sitting for long periods
Avoiding inactivity is especially important in cold weather, as joints stiffen more quickly when the body becomes sedentary.
3. Perform Proper Warm-Ups Before Any Exercise
Cold muscles are more likely to tighten and cause discomfort, so a thorough warm-up is essential before any physical activity, even light exercise.
A proper warm-up should include:
-
5–10 minutes of light aerobic movement
-
Dynamic stretches for the target muscle groups
-
Gradual progression from low to moderate intensity
Warming up increases tissue elasticity and reduces strain on joints, tendons, and ligaments.
4. Improve Posture and Ergonomics
Since many people stay indoors longer during colder seasons, maintaining proper posture is crucial. Long periods of slouching increase pressure on the spine, knees, and hips, leading to unnecessary joint stress.
Practical tips include:
-
Adjust chairs to support lower-back curvature
-
Keep screens at eye level
-
Ensure wrists are neutral when typing
-
Avoid crossing legs for extended periods
-
Use lumbar rolls or cushions when sitting for long amounts of time
Better ergonomics help maintain even weight distribution, reducing wear on the joints.
5. Maintain a Balanced Diet Rich in Anti-Inflammatory Nutrients
Nutrition plays a critical role in managing inflammation. A diet rich in anti-inflammatory foods helps support joint health and reduce flare-ups.
Helpful dietary components include:
-
Omega-3 fatty acids (fish, flaxseed, walnuts)
-
Vitamin D and calcium
-
Antioxidant-rich vegetables and fruits
-
Adequate protein for muscle support
Staying hydrated is equally important, as dehydration can reduce synovial fluid lubrication.
6. Manage Body Weight to Reduce Joint Load
Extra body weight puts significant pressure on weight-bearing joints, especially the knees and lower back. Maintaining a healthy weight helps reduce friction and stress on these areas.
Even small, consistent lifestyle changes—daily walks, improved nutrition, and reduced sugar intake—can make a meaningful difference over time, particularly in winter when weight gain is more common.
7. Use Protective Braces to Stabilize and Support Vulnerable Joints
Cold weather increases the risk of joint instability due to muscle stiffness and reduced tissue elasticity. This is why many clinicians recommend using orthopedic braces during colder months, especially for individuals with arthritis, chronic pain, or previous injuries.
High-quality braces can:
-
Provide stability and prevent excessive joint movement
-
Retain heat to improve circulation and reduce stiffness
-
Reduce stress on inflamed or weakened tissues
-
Improve posture and alignment during work or exercise
-
Enhance daily comfort and prevent flare-ups
Commonly used braces include:
-
Compression gloves for hand stiffness
-
Wrist braces for repetitive strain or RA flare-ups
-
Knee braces for osteoarthritis or sports injuries
-
Back braces for lumbar support during prolonged sitting
-
Shoulder and elbow braces for tendinitis or instability
-
Ankle and leg braces for weakness or balance issues
These devices are especially helpful for individuals working in physically demanding environments or those recovering from injury.
8. Consult Healthcare Professionals When Symptoms Persist
While seasonal joint discomfort is common, chronic or worsening pain should be evaluated by a healthcare provider. Medical professionals may recommend personalized treatment such as physiotherapy, targeted exercises, imaging tests, medication, or long-term support solutions.
How Cold Weather Aggravates Different Joints
Hands and Fingers
The small joints of the hands and fingers are particularly sensitive to temperature changes. As the weather becomes colder, blood vessels supply less warm blood to the extremities, which lowers joint temperature even further. For people who type frequently, perform repetitive hand work, or suffer from arthritis, the drop in joint temperature increases synovial fluid viscosity and reduces lubrication in the finger joints.
Cold-induced stiffness also weakens grip strength, making tasks such as holding tools, lifting objects, or even opening jars more difficult. Swelling can develop due to inflammatory responses, amplifying discomfort.
How to Manage It:
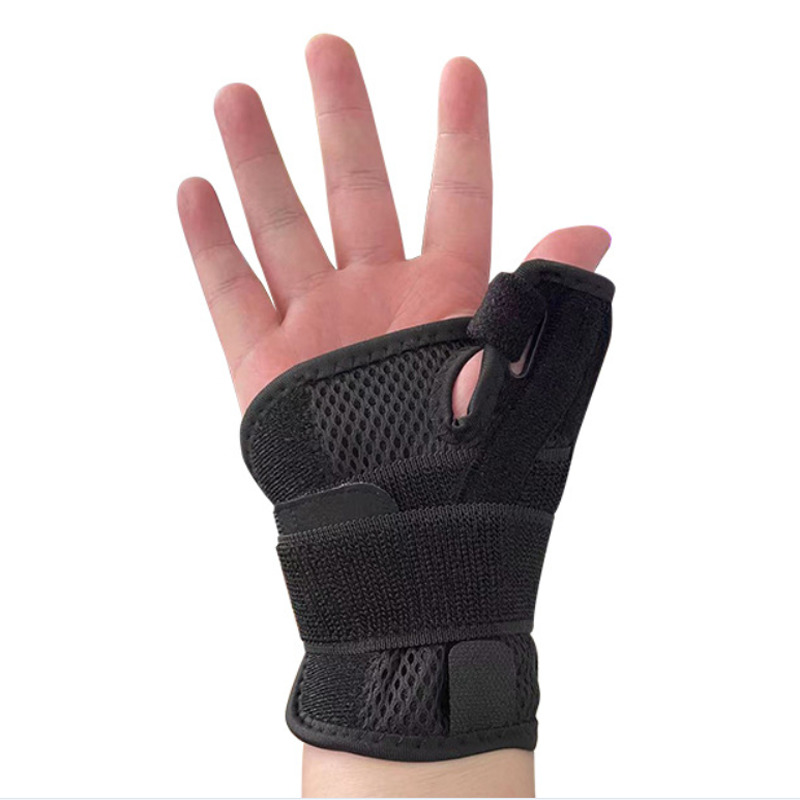
Compression Gloves manufactured by Wecare help retain heat, promote blood circulation, and reduce swelling. Their mild compression supports hand mobility, making them ideal for cold seasons or temperature-sensitive activities.
Wrists
The wrist contains multiple small bones, tendons, and synovial sheaths that can easily become irritated when the weather cools. Lower temperatures cause tendons to glide less smoothly, increasing friction—especially for people engaged in sports, typing, assembly-line jobs, or repetitive lifting.
People with carpal tunnel syndrome often report a significant increase in tingling, weakness, or stiffness in cold environments. This is largely due to reduced blood flow in the carpal tunnel area and heightened sensitivity of the median nerve.
How Wecare Helps:
Wecare Wrist Braces stabilize the joint, reduce tendon stress, and maintain warmth. This makes them beneficial for both daily use and workplace ergonomics during the colder months.
Shoulders
The shoulder is one of the most mobile and complex joints in the human body. In cold conditions, the muscles around the rotator cuff tend to tighten, reducing range of motion and increasing the risk of strains. People with old injuries or adhesive capsulitis (“frozen shoulder”) frequently experience more significant discomfort as temperatures drop.
Cold air can also irritate nerve pathways around the upper back and neck, causing referred pain into the shoulder region.
Support Solution:
Wecare Shoulder Braces provide warm compression, stabilize the joint, and support the rotator cuff, helping reduce stiffness and maintain mobility during cold seasons.
Lower Back
The lumbar region responds strongly to cold exposure. When the temperature decreases, the paraspinal muscles tighten reflexively to preserve body heat, leading to stiffness and reduced flexibility. People with disc herniation, spinal arthritis, or chronic muscular tension may find that cold weather worsens nerve-related pain or muscle spasms.
Additionally, the cold can exacerbate inflammation in the joints connecting the spine and pelvis, limiting movement and causing discomfort after standing or sitting for extended periods.
Helpful Support:
Wecare Back Braces stabilize the lumbar region, offer structural support, and preserve local warmth, making them ideal for individuals with chronic lower back pain or those performing heavy physical work in colder environments.
Knees
Knee joints are among the most commonly reported areas of cold-weather pain. As temperatures drop, synovial fluid thickens and cartilage loses some of its cushioning capability. This is particularly problematic for people with osteoarthritis, old sports injuries, or chronic cartilage wear.
Cold weather also reduces muscle elasticity, making the quadriceps and hamstrings more prone to tightness. When the muscles around the knee are stiff, the joint absorbs more mechanical stress, increasing pain levels during walking, climbing stairs, or bending.
Recommended Support:
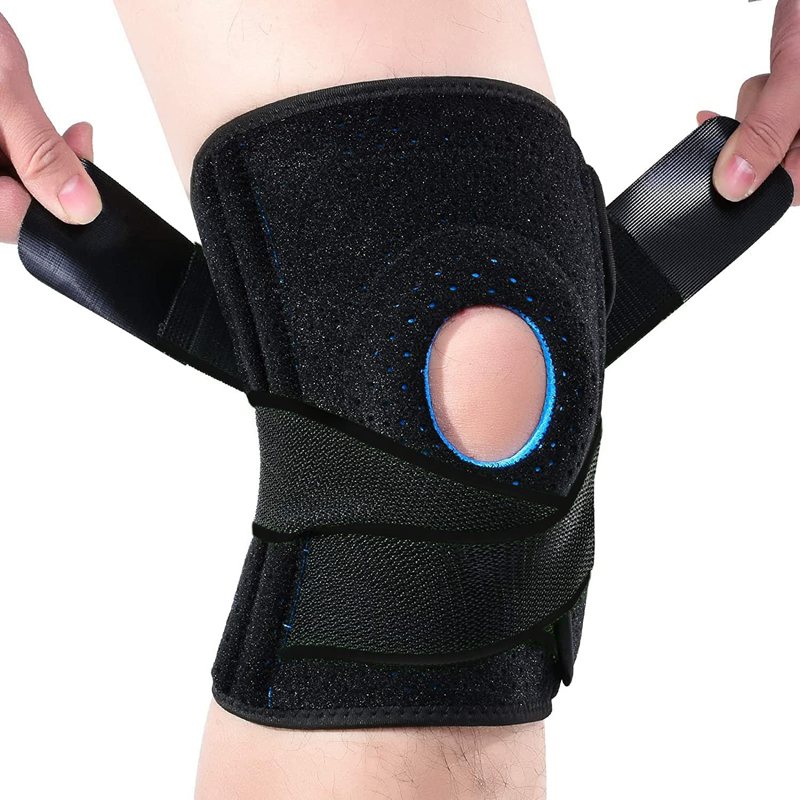
Wecare Knee Braces provide compression, improve proprioception, and help stabilize the joint. They reduce stress on the ligaments and maintain warmth, which is critical for knee mobility in cold conditions.
Ankles
Ankles are easily affected by cold, especially for individuals who have experienced sprains or instability. The ligaments around the ankle become less flexible in low temperatures, increasing the risk of micro-injuries. Cold can also aggravate tendonitis—particularly Achilles tendonitis—by reducing circulation and delaying tissue recovery.
For people who stand for long periods or participate in winter sports, swollen or stiff ankles are common due to both the temperature and increased load on the joint.
Optimal Management:
Wecare Ankle Braces help stabilize the joint, improve circulation, and maintain warmth, reducing the likelihood of instability-related pain during colder months.
Who Is Most at Risk for Cold-Induced Joint Pain?
Cold-related joint discomfort can affect anyone, but certain groups are significantly more susceptible due to underlying conditions, lifestyle demands, or previous injuries. Understanding the risk factors helps individuals prepare before temperatures drop and supports businesses in recommending practical protective solutions such as Wecare’s orthopedic braces and compression supports.
Individuals With Arthritis
People living with osteoarthritis, rheumatoid arthritis, or gout often experience heightened sensitivity to temperature changes. Cold weather increases joint stiffness, reduces circulation in affected areas, and triggers inflammatory responses.
Arthritis patients commonly report:
-
Morning stiffness lasting longer
-
Difficulty bending or straightening joints
-
Increased swelling
-
Tingling or burning sensations
Because arthritic joints already have reduced cartilage and compromised synovial lubrication, cold weather amplifies discomfort.
Those With Previous Joint Injuries
Old injuries—such as sprains, fractures, torn ligaments, or strained muscles—often flare up when the weather becomes cold. Scar tissue lacks the elasticity of healthy tissue and does not insulate well, making old injuries more sensitive to temperature drops.
People with past injuries may experience:
-
Increased stiffness
-
Sharp pain during movement
-
Instability in the joint
-
Weakness or limited range of motion
Using stabilizing supports like Wecare Knee Braces, Elbow Braces, or Ankle Braces helps protect vulnerable joints during cold seasons.
Outdoor Workers and Athletes
Those who spend long hours exposed to cold—construction workers, warehouse staff, delivery personnel, or winter athletes—naturally face higher risks. The constant temperature difference experienced when moving between warm and cold environments stresses tendons, ligaments, and joint capsules.
Athletes, especially runners or cyclists, often experience tightening in the lower body joints due to cold air and reduced warm-up effectiveness.
Wearing joint supports from Wecare offers:
-
Heat retention
-
Improved blood flow
-
Reduced risk of sprains
-
Enhanced overall movement comfort
Individuals With Poor Circulation
People with naturally low circulation, conditions like Raynaud’s, or metabolic disorders tend to experience exaggerated symptoms in cold weather. Reduced blood flow to the extremities causes joints to feel cold, stiff, or numb, and muscles fatigue more quickly.
Products such as Wecare Compression Gloves and Leg Braces can help improve circulation and reduce temperature sensitivity.
Aging Adults
As individuals age, synovial fluid thickens, cartilage becomes thinner, and muscle mass decreases. These changes make older adults especially prone to cold-induced joint pain.
Factors contributing to increased sensitivity include:
-
Slower tissue healing
-
Reduced flexibility
-
Higher prevalence of chronic joint diseases
-
Decreased balance and stability
Warm compression and structured bracing can significantly enhance comfort and mobility for older adults.
People With Sedentary Lifestyles
Sitting for long periods—such as office employees, drivers, or people working remotely—reduces joint lubrication and blood circulation. Cold indoor environments, air conditioning, or poor posture further increase stiffness.
Wecare’s Back Braces, Neck Braces, and Wrist Supports help maintain proper alignment and reduce cold-related discomfort from prolonged sitting.
Common Symptoms of Cold-Weather Joint Pain
As temperatures drop, the body responds in various ways that directly affect joint comfort and mobility. Recognizing the symptoms early allows individuals to take preventive measures—such as wearing Wecare’s orthopedic supports—to avoid worsening discomfort or long-term joint issues. Below are the most common symptoms experienced when the weather turns cold.
Increased Stiffness
Stiffness is one of the earliest and most noticeable symptoms of cold-induced joint discomfort. When temperatures fall:
-
Synovial fluid becomes more viscous
-
Muscles tighten to conserve heat
-
Blood flow decreases in the extremities
-
Connective tissues lose elasticity
These changes lead to a reduced range of motion, making tasks like bending, stretching, or gripping feel noticeably more difficult. Stiffness typically affects the hands, knees, and lower back more severely.
Aching and Deep Joint Pain
Cold temperatures often trigger deep, dull pain within the joints. This type of pain tends to occur:
-
After waking up
-
After prolonged sitting
-
During weather changes
-
While walking or climbing stairs
Atmospheric pressure drops may also contribute to discomfort, causing joint structures to expand or contract slightly. Individuals with arthritis frequently describe this as a “deep ache,” especially in weight-bearing joints like the hips, knees, and ankles.
Swelling or Mild Inflammation
Although cold temperatures typically reduce inflammation, some people experience swelling due to muscle tension, restricted circulation, or underlying chronic conditions. Swollen joints feel:
-
Warm or tender
-
Puffy or tight
-
Difficult to move
Compression-based products—such as Wecare Compression Gloves, Knee Braces, or Ankle Supports—can help manage swelling by improving circulation and stabilizing soft tissues.
Sharp or Shooting Pain During Movement
In some cases, joint pain becomes sharper and more intense during sudden movements. This may happen due to:
-
Tightened ligaments
-
Inflamed tendons
-
Nerve sensitivity
-
Old injuries reacting to the cold
The knees, elbows, and wrists commonly develop sharp pains when performing quick motions such as lifting, twisting, or stepping.
Reduced Grip Strength
Cold weather significantly affects hand dexterity. When the muscles and tendons in the fingers become stiff:
-
Grip strength decreases
-
Fine motor skills worsen
-
Typing, writing, or holding objects becomes uncomfortable
This is especially challenging for people who perform detailed manual tasks. Wecare Compression Gloves help retain warmth and provide gentle compression to maintain hand mobility.
Numbness or Tingling
Numbness and tingling occur when cold temperatures restrict blood flow or irritate nerve pathways. Common affected areas include:
-
Fingers
-
Toes
-
Wrists
-
Shoulders and neck
People with previous nerve-related conditions—such as carpal tunnel syndrome or cervical issues—are more prone to these sensations in cold weather.
Overall Weakness or Joint Instability
Cold muscles are less efficient and more prone to fatigue. As a result, individuals may notice:
-
Difficulty supporting body weight
-
Wobbliness around the knees or ankles
-
Fatigue during simple movements
-
Increased risk of sprains
Wecare’s line of Knee Braces, Ankle Braces, and Spinal Supports helps improve stability and reduce the risk of cold-season injuries.
Conclusion
As temperatures begin to drop, joint pain becomes a common challenge for individuals of all ages, especially those with arthritis, previous injuries, or physically demanding lifestyles. Cold weather reduces circulation, increases muscle tension, and thickens synovial fluid, all of which contribute to stiffness, swelling, and discomfort in major joints such as the hands, wrists, shoulders, back, knees, and ankles. Understanding these physiological responses is the first step toward effective prevention and long-term joint health management.
While cold-induced joint pain is difficult to avoid completely, it can be significantly reduced with proper protection, consistent movement, and the right supportive equipment. Warm compression, joint stabilization, and improved circulation all play crucial roles in maintaining comfort and mobility throughout colder months.
As a professional manufacturer of orthopedic supports and compression products, Zhengzhou Wecare Glove Company Ltd. is committed to helping global partners deliver reliable, high-performance solutions to their customers. With over seven years of production experience, CE and ISO-certified products, and a strong track record in OEM/ODM projects, Wecare offers a comprehensive range of products including Compression Gloves, Wrist Braces, Shoulder Braces, Back Braces, Elbow Braces, Neck Braces, Leg Braces, Knee Braces, Ankle Braces, and Spinal Braces.

_1763964804_WNo_1024d506.jpg)